(Last updated 9/6/2023)
The COVID-19 pandemic wreaked havoc in every aspect of life for over a year. The healthcare industry unsurprisingly bore the brunt of it. 2020 saw unprecedented declines in procedure volume and healthcare revenue. While the arrival of vaccines and prospects of herd immunity have given the first glimpse of the light at the end of the tunnel, how can providers ensure they reach it?
In this blog, we’ll look at the current state of healthcare revenues, ways to recover losses incurred from the onset of the pandemic, and ways to stop the leaks that allow more revenue to slip through the cracks.
Short on time? Watch the iPro Byte version of this blog for a short summary of key takeaways.

The State of Healthcare Revenue
This blog was originally published in March of 2021, a year after the pandemic began. The next section looks at the state of healthcare revenue at the start of 2021, as well as the outlook (at the time) for the rest of that year. New sections have been added to discuss how 2021 turned out and the state of healthcare revenue in 2022 and Q1 2023
2021
The start of the pandemic saw a drastic dip in procedure volume and revenues. In fact, total healthcare services spending in Q2 2020 was down nearly 9% from the same time in 2019. While Q3 and Q4 saw some moderate increase in revenues, total healthcare services spending in 2020 ended up being down 1% from 2019. Physician offices and ambulatory care centers saw the biggest losses: 3.8% and 2.7% respectively. While hospital revenue initially dipped 5.6% in Q2, the Q3 and Q4 gains resulted in a net increase of 0.1% compared to 2019.
While the incremental gains over the last few quarters of 2020 were encouraging, the outlook for 2021 was bleak. A study published by Kaufman Hall in February 2021 projected a further $53 billion loss in healthcare revenue in 2021 – under an optimistic scenario. This scenario assumed the following:
- Volume returned to pre-COVID levels
- Vaccines were distributed quickly and without significant delays
- COVID-19 cases steadily declined due to social distancing, masking, vaccination, etc. until herd immunity was achieved
Of the $53 billion loss in this optimistic scenario, nearly half ($27 billion) came from ambulatory care. Kaufman Hall also provided predictions for a pessimistic scenario. Assumptions for this scenario were:
- Volume slowly returned to partial pre-COVID levels
- Vaccine distribution was delayed
- COVID-19 cases surged cyclically due to non-compliance of social distancing measures before herd immunity was achieved.
Under this pessimistic scenario, hospital revenue loss was expected to be about $122 billion, with $64 billion coming from ambulatory care.
2022
Fortunately 2021 hospital revenues exceeded even the optimistic projections. According to a Kaufman Hall report released in January 2022, gross operating revenue was 14.7% higher in 2021 compared to 2020, and 12.1% higher compared to 2019. Outpatient revenues, which were some of the hardest hit in 2020, increased 18.5%. Operating margins also saw a median increase of 44.8% over 2020 excluding CARES Act funding.
While these revenue metrics are promising, hospitals are still mostly in a weaker financial position than they were before the pandemic. While Operating Margins in 2021 were much higher than 2020, they were still down 3.8% from 2019 without CARES funding. This is largely due to increased expenses, particularly labor expenses. For instance, Labor Expense per Adjusted Discharge was 4.6% higher in 2021 than 2020 and a whopping 19.1% higher than 2019. This is due largely to staff shortages and COVID-19 surges.
2023
According to a January 2023 Kaufman Hall report, 2022 ended up being the worst financial year for hospitals since the start of the pandemic. While net operating revenue was up 15% from 2021, profitability was down a whopping 30%. Kaufman Hall attributes this largely to increased labor expenses and increased lengths of stay. To overcome these challenges, Kaufman Hall recommends:
- Better workforce management strategies
- Securing more stable supply lines
- Effectively negotiating with payers
- Leveraging outpatient footprint and improving relationships with post-acute settings
Recovering Losses and Preventing Leakage
Now that we’ve examined the state of healthcare revenue and seen there’s still a steep hill to climb, let’s look at some ways hospitals can recover losses incurred by the pandemic.
Encouraging Consumers
As noted in Kaufman Hall’s optimistic scenario projections, a return to pre-pandemic volumes is key to recovering revenues. One of the best ways to encourage consumers to seek in-person care is by reassuring them your facility is following proper COVID-19 safety measures. Ways to promote your facility’s safety mindfulness include:
- Listing the steps you’re taking to ensure a safe, clean environment on your website for patients to view ahead of time
- Posting COVID-19 safety reminders (i.e. social distancing, masking, sanitizing, etc.) at all entrances
- Providing patients with vaccine information, such as how vaccines work and how/where to get vaccinated
- Encouraging vaccinated staff to wear stickers showing they’ve been vaccinated
These are just some of the steps you can take to encourage consumers to return to in-person care. In addition to encouraging consumers to come to your facility, encouraging them to get vaccinated can also help volume and revenue levels to return to pre-pandemic levels faster. Check out the AMA’s 10 tips for talking to patients about vaccines to get started.
Engaging Patients
Creating, or improving, patient loyalty is also critical to recapturing lost revenue. Loyal patients will feel more comfortable going to your facility for treatment and are also likely to recommend it to their friends and family. While there are many ways to create, maintain, and improve patient loyalty, the key is to engage patients throughout the care journey. This often starts before the patient even sets foot in your facility, makes the first call, or sends the first email.
In the digital age, your online presence is often the first encounter a patient will have with you. While some aspects of your web presence are out of your control, such as online reviews, your own website can have a significant impact on a consumer’s decision. A professional, clean-looking website with simple navigation and helpful links and resources can make a great first impression.
Your website can also serve as the hub for your entire digital front door strategy. From the patient portal to navigation resources, to follow-up communications, engaging patients every step of the way is vital to maintaining patient loyalty and generating more revenue.
Enhancing Offerings
Encouraging consumers to return to in-person care and engaging them throughout the care process are great ways to build loyalty and capture more patients through word of mouth. While these tactics can certainly boost healthcare revenues, providers should also strive to enhance their offerings.
If there’s one thing the pandemic has taught us, it’s that the healthcare industry needs to continually evolve to stay prepared for the next big catastrophe that could strike at any moment. While the industry is notorious for slow advancement, 2020 showed that it is indeed capable of kicking it into high gear when pushed to the brink.
Enhancing your facility’s offerings not only ensures it’s well-prepared to handle what’s to come, but it can also serve as a competitive advantage. If your facility offers services other local providers don’t, or if you invest in tech that streamlines care and/or improves the patient experience, you’ll attract more patients and more referrals. Some enhanced offerings to consider are:
- Clinical decision support to ensure the right exams are ordered for the right patient
- Patient transportation services
- Payment assistance or other flexible payment options such as 0% interest payment plans
- Procedure instructions/videos
- Remote monitoring devices
- Scheduling assistance, including appointment reminders and navigation assistance/instructions
There are many ways to enhance your offerings and capture more revenue. You don’t have to invest in all of them, but you can be sure your competitors will be looking to enhance their offerings as well.
Enlarging Your Referral Base
As we touched on in the previous tip, enhancing your offerings can lead to more referrals from physicians and specialists. This leads us to our next tip for recovering lost healthcare revenue and preventing leakage: enlarging referrals. It’s simple – more referrals = more money.
The great thing is that by following the previous suggestion of enhancing your offerings, you’re already giving referring providers more reasons to send patients to your facility. Other ways to increase referrals include physician outreach programs (i.e. emails, flyers) and physician onboarding initiatives such as training sessions that familiarize physicians with your procedures and systems.
To learn more about preventing revenue leakage from lost referrals, download our whitepaper.
Minimizing Claim Denials
Another source of healthcare revenue loss is denied claims, with an average of 10% of claims denied each year upon initial submission. A recent study by Change Healthcare concluded that 86% of denied claims are preventable. Additionally, over half of denied claims are due to issues on the front-end of the revenue cycle. Top reasons for claim denials include:
- Authorization and pre-certification issues
- Eligibility and registration issues
- Medical coding errors
- Medical necessity issues
- Missing claims
- Uncovered services
By addressing these issues, providers can minimize claim denials and prevent revenue loss. Fortunately, these issues can all be addressed on the front end when a medical order is placed. Ambulatory order management is an often overlooked part of the revenue cycle. An order management solution with an integrated clinical decision support mechanism (qCDSM), like iOrder, can help ensure a claim will be paid before the order is even submitted. Improving the prior authorization process can also ensure claims are paid on-time and care isn’t delayed. Our iOrder solution offers integration with prior authorization specialists AuthNet to remove the burden of prior authorizations from your staff. To learn more about how iOrder can help minimize claim denials and maximize reimbursement, request a free demo today.
The below National Association of Healthcare Revenue Integrity (NAHRI) podcast goes into more detail on the importance of ambulatory order visibility on the revenue cycle.

For more tips on maximizing reimbursement and growing revenue, check out our blog on overcoming 3 major reimbursement challenges.
Mitigating Burnout
A significant source of healthcare revenue leakage is provider burnout. How much does burnout cost hospitals exactly? A 2018 report by the American Medical Association (AMA) estimated burnout costs hospitals between $500,000 and $1 million per doctor. This is due to the costs of recruitment and/or replacement when a burned out physician takes time off or leaves altogether. Burnout also causes inattentiveness and frustration, which leads to medical errors and malpractice, costing hospitals even more money. Keep in mind, this is the cost for only one burned out physician. The AMA report highlighted a scenario in which a facility could lose as many as 60 physicians over a 2 year period, resulting in costs between $15.5 to $55.5 million!
On top of these costs, there’s the actual revenue leakage in the form of lower productivity resulting in fewer patients seen and patient dissatisfaction as a result of a decline in quality. These two factors could result in lost patient care. Whether a patient is put off by a burned out caregiver’s demeanor or the noticeable lack of experience in a younger replacement, one negative experience can significantly damage a hospital’s relationship with a patient. This damage could be compounded by negative word of mouth.
At a time when patients are just beginning to feel comfortable returning to in-person care, the last thing you want is for them to have a bad experience due to clinician burnout. After all, your patient revenue loss is your competitors’ gain.
Now that you know how serious a financial problem burnout is, learn what clinicians are saying about it and how to mitigate it.
The Road to Relief
The COVID-19 pandemic has put a financial strain on many industries. The healthcare industry has been one of the primary victims. 2020 saw significant declines in healthcare revenue, and more major losses are expected this year in even the most optimistic scenarios.
That’s why it’s important for providers to make every effort to recover revenue where they can, capture new revenue to make up for their losses, and prevent further revenue leakage. As a refresher, the six strategies we covered in this blog are:
- Encouraging Consumers
- Engaging Patients
- Enhancing Offerings
- Enlarging Referrals
- Minimizing Claim Denials
- Mitigating Burnout
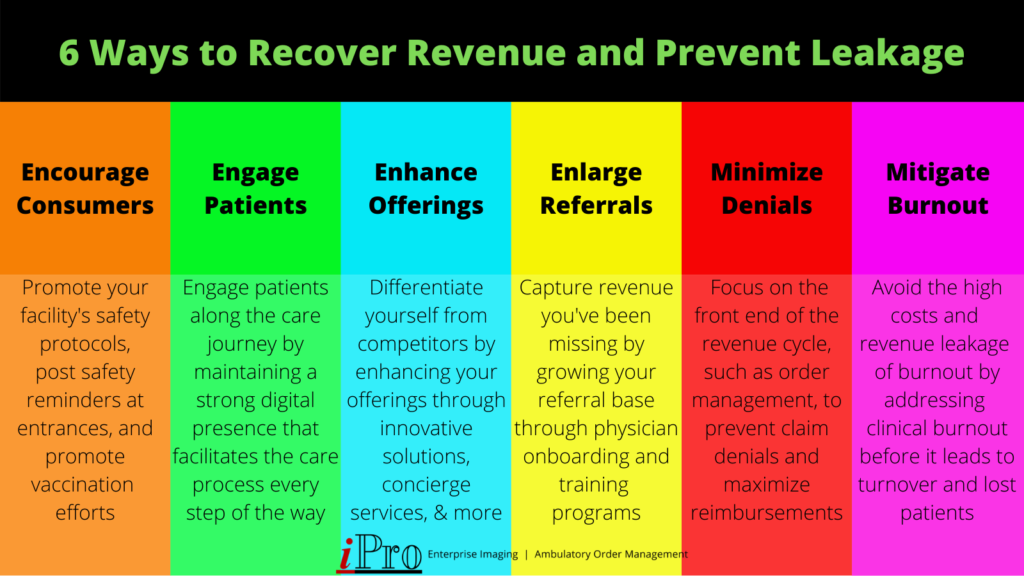
There are certainly more ways to bounce back from the financial losses brought on by the pandemic, but these six provide a comprehensive approach to bring in revenue and prevent it from leaking out.
An often overlooked area of the revenue cycle is order management. As we discussed in the “Minimizing Claim Denials” section, proper order management can play a significant role in recovering revenue by maximizing reimbursements. The benefits don’t end there though. Order management touches all six areas of revenue recovery we previously discussed.
For more tips on optimizing revenue through order management and patient scheduling, download our new eBook “A Revenue Cycle Leader’s Guide to Patient Scheduling for Maximum Impact“.
To learn how our ambulatory order management solution, iOrder, can improve your revenue cycle, watch this short video or contact us today.





