It’s hard to believe we’re already halfway through 2021. While 2020 was dominated by the COVID-19 pandemic, this new year has seen a gradual return to normal due to the advent of vaccines. In this blog, we’ll discuss the state of healthcare in 2021 so far, from vaccine rollouts to innovations in health tech to the challenges facing the healthcare industry post-COVID.
Vaccines
Perhaps the biggest story in the state of healthcare so far in 2021 is the rollout of COVID-19 vaccines. In the first few months, vaccines were available in the U.S. to only certain groups, such as the elderly, immunocompromised, and frontline health workers. As vaccine production and supply increased, access has expanded to everyone.
By mid-June, over 300 million doses of the vaccine had been administered in the U.S., however, only 45% have been fully vaccinated. While COVID-19 restrictions have been greatly reduced or lifted entirely in most states, vaccination rates have been dwindling with the daily average number of Americans receiving their first dose falling from 500,000 to 200,000 – a 60% decrease. At the time of writing, 65% of U.S. adults have received at least their first dose of the vaccine, which puts President Biden’s goal of 70% of adults having received their first dose by July 4th in jeopardy.
According to a recent survey, 97% of vaccinated Americans plan to travel this year. The majority of respondents (51%) said they would be most likely to travel for a family event, such as a wedding, while 33% said they would be most likely to plan travel for the 4th of July. As COVID-19 variants continue to emerge, vaccination efforts will likely increase, with the government, corporations, and even physicians themselves working to educate citizens on the safety and efficacy of vaccines and dispel myths and conspiracies.
Healthcare Innovations
The pandemic has also led to some new innovations in healthcare. For instance, California is now offering digital vaccine records. Realizing that vaccinated people may misplace their physical vaccine card, the state has launched a digital platform where people can show proof of vaccination via PIN or QR code on their mobile phone. A recent Becker’s Healthcare article featured some of the most promising healthcare tech in 2021 according to 13 healthcare executives, many of which came out of the pandemic. Among the technologies featured were:
- AI diagnostic tools
- Analytics software
- Machine learning
- Remote monitoring tech
- Self-scheduling tools
- Telehealth
- Voice technology
Not all innovations are COVID-related though. A recent innovation that’s generated a lot of discussion is Aduhelm, Biogen’s Alzheimer’s drug approved by the FDA on June 7th. Not only is Aduhelm the first FDA-approved Alzheimer’s treatment sent 2003, it’s also the first FDA-approved treatment intended to slow cognitive decline, as opposed to merely alleviating symptoms. Aduhelm’s approval has been met with mixed reactions however. According to a recent survey, 80% of pharmaceutical workers disapprove of the drug’s approval. The FDA has said it will continue to monitor the drug as it is administered to patients.
Challenges Post-COVID
While the COVID-19 pandemic itself has been a monumental challenge, it has also given rise to additional hurdles providers must face. Among these are recovering revenues lost due to COVID-19, managing increased patient and procedure volumes as normal levels return, and dealing with the health consequences of postponed care and treatment.
Recovering Revenue
It’s no secret that the pandemic has had a tremendous effect on healthcare revenues. In one of our recent blogs, we took a deep dive into 6 ways to recover revenues and stop further leakage. The 6 strategies we discussed in that blog were:
- Encouraging patients to return for care & treatment by assuring them proper safety measures were in place
- Engaging patients along the care journey through the use of a comprehensive digital front door and patient engagement strategy
- Enhancing existing services and expanding offerings with innovative tech, such as clinical decision support mechanisms, patient navigation assistance, and patient transportation services
- Growing referrals by strengthening relationships with referring physicians
- Minimizing claim denials by ensuring order accuracy and PAMA compliance, and
- Mitigating burnout
Implementing revenue recovery strategies is only part of the solution though. You also need to use the right technology. At iPro, our award-winning ambulatory order management solution, iOrder, can help your revenue recovery efforts across all six areas discussed above. Watch the video below to learn more about how iOrder can improve your revenue cycle:
Managing Increased Patient & Procedure Volumes
Another challenge facing healthcare providers is the rapid increase in patient and procedure volumes as people become more comfortable seeking medical care. At the height of the pandemic, U.S. healthcare providers saw an average decrease of 35.2% in CMS-defined shoppable services. In some states, this drop in volume was even starker. Massachusetts saw the largest decline, a whopping 48.5% decrease from the same period in 2019.
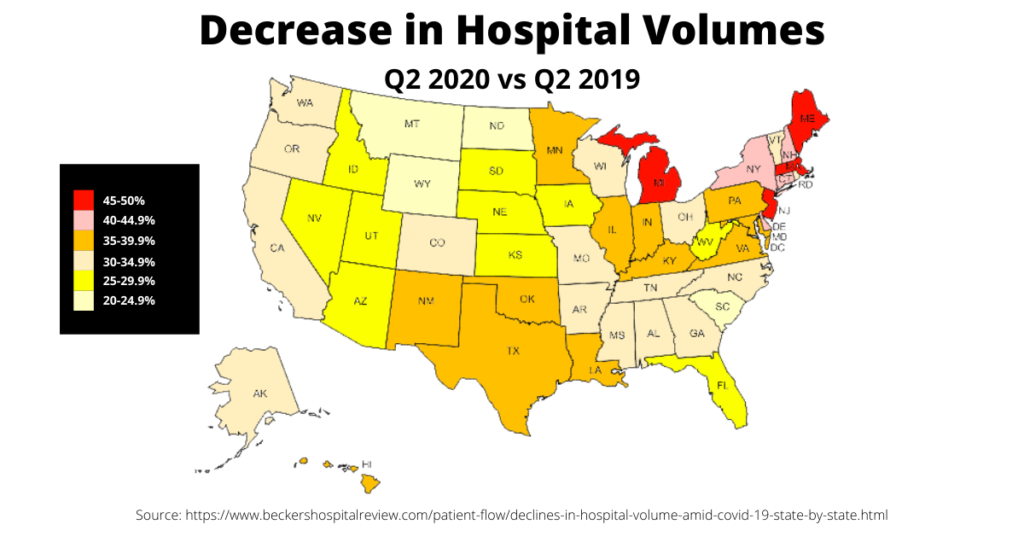
As vaccination rates have risen and daily COVID-19 cases have substantially declined however, patients are returning for care, particularly for outpatient care. Through April 2021, outpatient volumes have been higher each month compared to both 2020 and 2019. In fact, March 2021 volumes were a staggering 36.8% higher than March 2019, compared to a 58.9% decrease at the start of the pandemic in March 2020.
This influx in patient volume has resulted in a healthcare hiring spree, with healthcare employment in May returning to December 2020 levels. Of the 22,500 healthcare jobs added in May, 22,000 were in ambulatory services. However, healthcare employment is still down 3.1% from its February 2020 peak, and even ambulatory care jobs are still below pre-pandemic levels despite the large gains in May. The steady rise in healthcare employment the past few months doesn’t appear to be keeping up with the patient volume increases though. This has led to public complaints among healthcare professionals.
As patient volumes continue to climb, providers will need to get creative in regards to hiring and retaining employees. Tactics to consider include:
- Pay raises
- Mental health/burnout resources for staff
- Tech that streamlines/reduces workflows
Consequences of Delayed Care
While patients are beginning to seek out care again, including routine checkups, many in the healthcare field are concerned with the effects from the months of delayed care during the height of the pandemic. Putting off routine checkups can lead to undiagnosed ailments, and by the time a patient decides it’s safe to undergo that checkup, an undiagnosed disease may have progressed significantly. The same is true for delayed follow-up care post-diagnosis and postponed surgeries.
Of course, providers can’t accommodate all these patients returning at once, which leads to backlogs and further delays. Recent studies have also indicated that patients diagnosed with COVID-19 experience higher post-operative death rates even weeks after their diagnosis. Thus, the increased risk of death and other complications following elective procedures for COVID-19 patients results in even more delayed care. This sharp increase in delayed care is why the National Cancer Institute is projecting 10,000 excess deaths due to breast and colorectal cancer alone over the next decade. While this is only a 1% increase, it’s a startling number and representative of only two types of cancer. The total number of excess deaths due to delayed care is likely to be much higher.
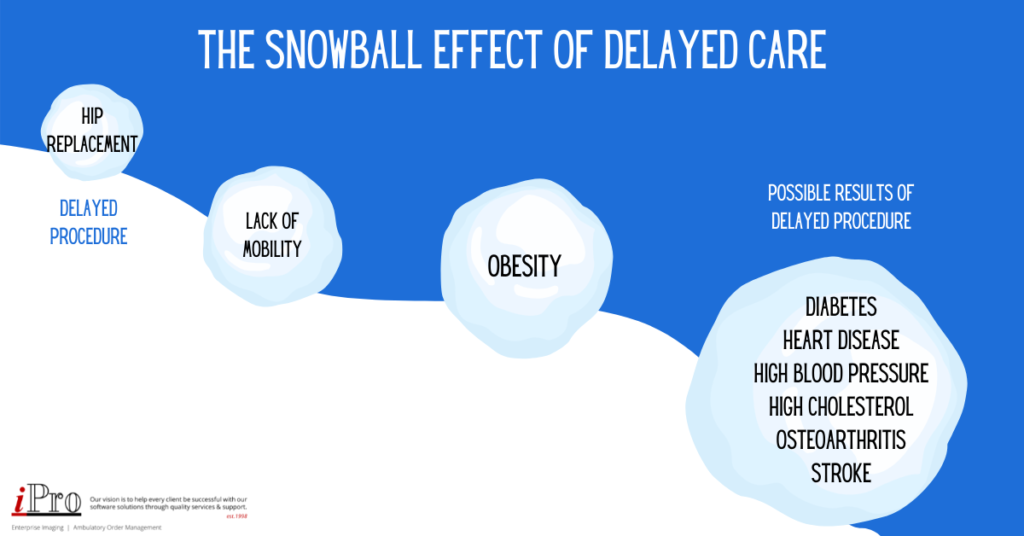
Excess deaths aren’t the only issue of delayed care though. The postponement and repeated cancelations of elective surgeries, such as hip replacements, can prolong a patient’s discomfort and lower their quality of life. Unresolved health problems can compound, leading to more health issues down the road. For instance, if a patient’s hip replacement surgery keeps getting delayed, their mobility will continued to be limited. This hinders their ability to exercise, which in turn increases their risk of obesity and a host of other medical problems that come with obesity. The constant pain or discomfort and stress can also have adverse mental health effects. It’s easy to quantify the deaths directly caused by COVID-19, but the indirect deaths and maladies may only be revealed over time.
To learn about more healthcare challenges providers are currently facing and some tech that can help overcome them, read our recent blog.
The Road Ahead
The state of healthcare halfway through 2021 is still strongly tied to the COVID-19 pandemic. Most of the top healthcare stories so far this year – vaccines, healthcare innovations, and new challenges – are born out of the pandemic. In fact, COVID-19 is likely to continue influencing our daily lives, especially in healthcare, for years to come.
As for the months ahead, much may depend on vaccination rates. If rates continue to dwindle, pockets of COVID-19 surges may pop up in areas with lower vaccination rates, especially as the number of COVID-19 variants continues growing. In areas with higher vaccination rates, a return to pre-pandemic operations is more likely. No matter how “normal” things get however, COVID-19 is sure to have a long-lasting effect on the world through healthcare innovations, long-term direct and indirect health effects, and how providers prepare for future pandemics.
At iPro Healthcare, we’ve been helping our clients achieve their goals for over 20 years. As you navigate post-COVID challenges such as recovering revenue and managing increase ambulatory volumes, we’re here to help.
To learn more about how our iOrder solution can help improve your ambulatory order processes, streamline workflows, strengthen relationships with referring providers, and minimize claim denials, contact us today.




